The medical billing industry is undergoing a massive digital evolution. The transition from manual, paper-based processes to electronic systems is no longer just about adopting new technology; it is about eliminating administrative bottlenecks so you can shift your focus back to patient care. At the heart of this transformation is Electronic Data Interchange (EDI). For healthcare providers across the US, mastering EDI is the ultimate key to optimizing your financial health, securing your revenue cycle, and streamlining operations.
At Quick RCM (www.quickrcm.com), we know that navigating the complexities of medical billing, coding, and Accounts Receivable (AR) can be overwhelming. This comprehensive guide will explore the digital backbone of modern medical billing EDI systems, how they transform the healthcare revenue cycle, and why outsourcing your RCM to our expert team can maximize your practice’s profitability.

What is Electronic Data Interchange (EDI)?
Electronic Data Interchange (EDI) is the secure, standardized, computer-to-computer exchange of healthcare information. It actively replaces outdated, error-prone methods like physical mail, faxes, and manual data entry. By adhering to strict, HIPAA-regulated layouts, EDI ensures consistent and secure communication between medical practices, clearinghouses, and insurance payers.
When information is exchanged electronically, it removes the roadblocks that have historically hindered effective healthcare management, offering precision and immediacy instead of uncertainty and payment delays.
The Core EDI Transactions Explained
To fully leverage EDI in your Revenue Cycle Management (RCM) strategy, you must understand the specific transaction types that facilitate communication. HIPAA regulates these standardized formats to ensure uniformity across the healthcare industry:
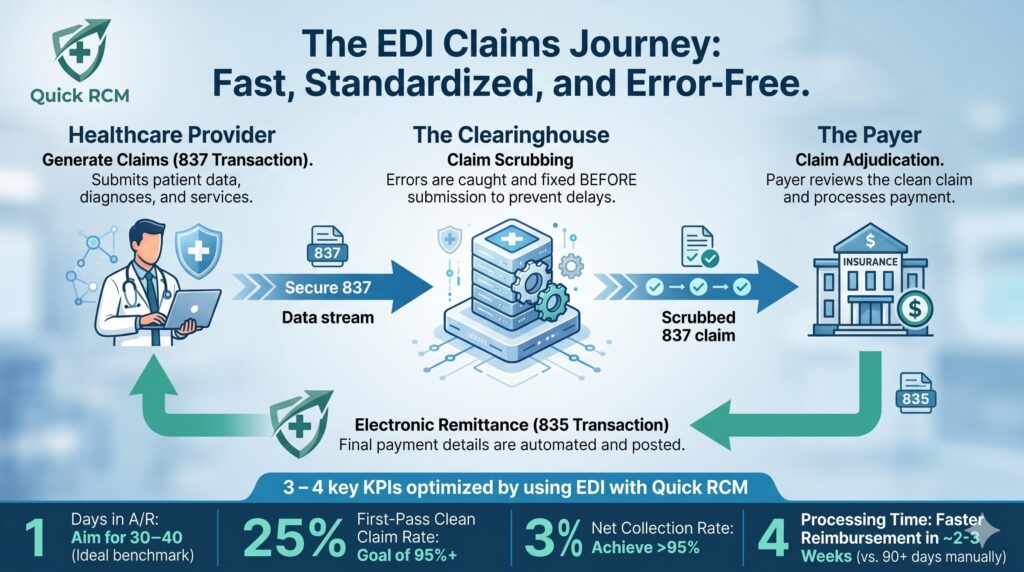
- 837 Transactions (Claim Submissions): This is the electronic format used to submit healthcare claim billing information. It holds critical details about the medical services provided, the specific diagnoses (ICD-10 codes), the procedures performed (CPT/HCPCS codes), and practice information.
- 270/271 Transactions (Eligibility Verification): Before a patient even walks through the door, Verification of Benefits (VOB) should occur. The 270 transaction is the inquiry sent to the payer, and the 271 is the response confirming a patient’s active coverage, co-pays, deductibles, and co-insurance. Neglecting this step contributes heavily to revenue loss, as up to 15% of all claim denials stem from incorrect eligibility verification.
- 278 Transactions (Pre-Authorization Requests): This EDI format is used to request authorization from an insurance company before specific procedures are performed. Failing to secure prior authorization leads to costly CO-15 or CO-197 denials, which completely halt your reimbursement.
- 276/277 Transactions (Claim Status): Instead of spending hours on hold with insurance companies, billing staff use the 276 inquiry to check claim status, receiving a 277 response detailing exactly where the claim stands in the adjudication process.
- 835 Transactions (Electronic Remittance Advice): This EDI request provides complete payment details from the payer, detailing approved amounts, contractual adjustments, and denial reasons.
Deep Dive: ERA vs. EOB
The 835 transaction, or Electronic Remittance Advice (ERA), has revolutionized the payment reconciliation process. It is important to understand how an ERA compares to the traditional Explanation of Benefits (EOB).
An EOB is a paper document sent via mail, summarizing claim outcomes and patient responsibility. It is slow, sometimes taking up to 90 days to reach the patient, and requires manual input into billing software, making it highly susceptible to human error.
Conversely, an ERA is a digital file (ANSI 835 format) transmitted securely and quickly, often within two to three weeks of claim filing. ERAs allow for automated claim posting directly into billing software, saving physical space, minimizing data entry errors, and dramatically speeding up the reconciliation of your Accounts Receivable.
The EDI Workflow: Clearinghouses and CPID
How exactly does an EDI claim travel from your practice to the payer? It rarely goes directly. Most healthcare practices use a clearinghouse as a secure intermediary.
Once a claim (837 transaction) is generated, it is routed to the clearinghouse. The clearinghouse “scrubs” the claim for any potential errors or missing data, allowing medical billers to make corrections before the claim ever reaches the payer’s system. This scrubbing process is your first line of defense against denials.
To ensure the claim reaches the correct destination, it relies on a CPID (Claim Payor Identification) number. A CPID acts like a digital address, accurately identifying the insurance payer so the clearinghouse can route the file correctly. Once the payer receives the EDI file, they adjudicate the claim and transmit their 835 ERA response back through the clearinghouse to your practice.
Hospital vs. Physician Billing in EDI
When setting up EDI connections, it is critical to understand the dichotomy between institutional (hospital) and professional (physician) billing.
- Hospital Billing (Institutional): This covers facility-based services, including room and board, operating room fees, and hospital laboratory tests. These claims are submitted using the UB-04 form, which is digitally transmitted as an 837-I transaction. Institutional EDI relies heavily on four-digit revenue codes (e.g., 0450 for the Emergency Room, 0360 for the Operating Room) alongside ICD-10 diagnosis codes.
- Physician Billing (Professional): This covers the clinical services provided by individual doctors, surgeons, or specialists in both inpatient and outpatient settings. These claims use the CMS-1500 form, transmitted as an 837-P transaction. Professional EDI focuses on CPT and HCPCS codes to detail the specific medical procedures and supplies utilized.
At Quick RCM, our systems seamlessly manage the unique EDI requirements for both 837-I and 837-P transactions, ensuring clean submissions regardless of your practice’s structure.
Decoding J-Codes and Revenue Codes in EDI
To maximize reimbursements, your EDI transmissions must carry the most precise medical coding available.
- J-Codes: These HCPCS Level II alphanumeric codes are essential for billing non-orally administered medications, biologicals, chemotherapy drugs, and injectables (e.g., J3420 for Vitamin B-12 injections). When transmitting 837 claims, J-Codes must strictly align with the National Drug Code (NDC) and include exact dosage units; otherwise, the payer’s EDI system will automatically reject the medication charge.
- Revenue Codes: Primarily used in 837-I institutional claims, these codes tell the payer where a service was performed and what type of resource was used. For example, Revenue Code 250 designates general pharmacy charges, while 300 indicates laboratory services. Revenue codes must be paired with the correct CPT/HCPCS procedure codes on the same line item to successfully pass through the clearinghouse’s EDI scrubber.
Combating Medical Billing Denials with EDI
Even with EDI, medical billing remains a maze of complex coding rules and rigid payer policies. Denials are a massive challenge, costing the healthcare industry billions, with each denied claim costing between $25 to $118 to rework and resolve. Integrating robust EDI systems and expert RCM services helps tackle the most common denial codes head-on:
- CO-29 (Timely Filing Expired): This denial occurs when a claim misses the payer’s strict submission deadline. EDI ensures rapid electronic submission, drastically reducing the risk of claims aging past filing limits.
- CO-50 (Medical Necessity): Payers deny claims if they deem a procedure investigational or not medically necessary for the patient’s condition. Proper EDI documentation and specific ICD-10 coding support your clinical justification.
- CO-15 & CO-197 (Missing Prior Authorization): The 278 EDI transaction ensures authorization is requested, approved, and documented digitally, preventing these frustrating administrative denials.
- OA-23 (Coordination of Benefits): When patients have multiple insurance plans, secondary payers require the primary payer’s ERA data. EDI streamlines the attachment of primary payment data to secondary claims.
- CO-236 (Unbundling): Triggered when incompatible procedure codes are billed together, violating National Correct Coding Initiative (NCCI) edits. Advanced EDI claim scrubbers automatically catch code incompatibilities prior to submission.
- CO-252 (Missing Documentation): Denied because a required attachment or medical record is missing. Modern EDI systems help automate the tracking and electronic submission of necessary clinical notes.
Credentialing: The Prerequisite to Successful EDI
Before any 837 claims can be successfully processed, healthcare providers must navigate the complex world of insurance credentialing. Credentialing is the rigorous process of verifying a provider’s qualifications, including education, licenses, and background checks, allowing them to join an insurance payer’s network.
Submitting EDI claims without proper credentialing will paralyze your cash flow. For example, if a new physician begins seeing patients before their enrollment is fully active, the payer will instantly deny every EDI claim with a “provider not found” error, trapping tens of thousands of dollars in unpaid revenue. Re-credentialing is also required every two to three years to maintain active status. Quick RCM manages this tedious administrative burden, ensuring your providers are fully paneled so your EDI transactions flow smoothly from day one.
The Crucial Role of Medical Billing Reporting
A robust EDI system generates massive amounts of data. To optimize healthcare revenue, this data must be transformed into actionable insights through essential medical billing reporting. Key reports include:
- Denial Reports: These reports track 835 ERA transactions to highlight which claims are rejected and exactly why. Analyzing these patterns allows practices to fix root causes and improve first-pass acceptance rates.
- Aging (Accounts Receivable) Reports: A/R reports provide a snapshot of unpaid balances categorized by payer and the age of the debt (e.g., 0-30, 31-60, 90+ days). They are vital for prioritizing aggressive AR recovery efforts.
- Procedure Code Utilization Reports: By analyzing 837 claim data, these reports track how often specific CPT codes are billed and how much revenue they generate, identifying your most profitable services.
- Productivity & Financial Reports: These offer a full view of your practice’s financial health, tracking the efficiency of billing staff and generating comprehensive profit and loss statements.
Key RCM Metrics Optimized by EDI
To guarantee financial success, healthcare providers must leverage the data generated by EDI systems to track Key Performance Indicators (KPIs).
- First-Pass Clean Claim Rate: The industry benchmark is a clean claim acceptance rate of 95% or higher. High first-pass rates mean faster reimbursements and significantly less rework.
- Days in Accounts Receivable (A/R): The average time to collect payments should ideally sit between 30 and 40 days. If A/R exceeds 60 or 90 days, it signals severe bottlenecks in claim processing.
- Net Collection Rate: This measures the amount collected versus the amount legally contracted to be paid. A healthy practice should aim for a net collection rate over 95%.
- Cost to Collect (CTC): The money spent on administrative staff and billing operations should ideally remain between 3% and 6% of your total revenue.
The Power of AI and Automation in EDI Systems
As we look toward 2026, the integration of Artificial Intelligence (AI) and automation with EDI is transforming how medical billing operates. Predictive automation now works quietly in the background, scanning EDI claims to catch missing documents, eligibility gaps, and risky codes long before submission.
AI algorithms analyze historical denial patterns, identifying root causes and suggesting corrective actions to prevent future rejections. Furthermore, Robotic Process Automation (RPA) bots can post payments and process 270/271 eligibility transactions in seconds with incredible accuracy.
While AI is immensely powerful, it cannot entirely replace human expertise. Skilled medical billers and coders are essential to interpret complex medical records, handle nuanced appeals, and ensure compliance with shifting payer regulations. The future is a hybrid model where AI handles repetitive EDI data exchange, empowering human experts to focus on complex denial resolution and strategic revenue growth.
Optimize Your RCM with Quick RCM
Managing EDI transactions, tracking changing CPIDs, fighting complex denials, and keeping up with evolving compliance rules is an overwhelming task. When healthcare providers attempt to manage billing in-house, they face high overhead costs for staff salaries, software licensing, and constant training. Furthermore, multitasking internal staff can lead to higher error rates, delayed claim submissions, and mounting Accounts Receivable.
This is where Quick RCM steps in. At www.quickrcm.com, we provide comprehensive, end-to-end Revenue Cycle Management services tailored to healthcare providers across the US.
- Full RCM Services: We manage the entire lifecycle of your claims, from initial 270/271 eligibility verification to final 835 payment posting.
- Advanced Denial Management: Our experts aggressively tackle CO-15, CO-50, and OA-23 denials, turning rejections into revenue through meticulous appeals and root-cause analysis.
- Expert Medical Coding: Our certified coders ensure accurate CPT, ICD-10, and modifier application, preventing NCCI unbundling errors and maximizing your allowable reimbursement.
- Aggressive AR Recovery: We clean up aged receivables, persistently following up with payers to ensure you get paid for every service rendered.
By outsourcing to Quick RCM, you eliminate the massive overhead of an in-house billing department, reduce your cost to collect, and benefit from a dedicated team focused solely on your financial health.
Embracing the full capabilities of EDI in medical billing is not just about regulatory compliance; it is about building a robust, digital infrastructure that guarantees stability and growth for your healthcare practice


